Intermittent Energy Restriction and Weight Loss a Systematic Review
- Review
- Open Access
- Published:
Intermittent versus continuous energy restriction on weight loss and cardiometabolic outcomes: a systematic review and meta-analysis of randomized controlled trials
Journal of Translational Medicine volume 16, Article number:371 (2018) Cite this article
Abstruse
Background
This systematic review and meta-analysis summarized the almost recent evidence on the efficacy of intermittent energy restriction (IER) versus continuous energy restriction on weight-loss, body composition, blood pressure and other cardiometabolic gamble factors.
Methods
Randomized controlled trials were systematically searched from MEDLINE, Cochrane Library, TRIP databases, EMBASE and CINAHL until May 2018. Upshot sizes were expressed as weighted hateful deviation (WMD) and 95% conviction intervals (CI).
Results
Eleven trials were included (duration range viii–24 weeks). All selected intermittent regimens provided ≤ 25% of daily energy needs on "fast" days simply differed for type of regimen (5:2 or other regimens) and/or dietary instructions given on the "feed" days (ad libitum energy versus counterbalanced free energy consumption). The intermittent approach determined a comparable weight-loss (WMD: − 0.61 kg; 95% CI − 1.70 to 0.47; p = 0.87) or percent weight loss (WMD: − 0.38%, − 1.16 to 0.twoscore; p = 0.34) when compared to the continuous approach. A slight reduction in fasting insulin concentrations was evident with IER regimens (WMD = − 0.89 µU/mL; − i.56 to − 0.22; p = 0.009), only the clinical relevance of this result is uncertain. No between-artillery differences in the other variables were found.
Conclusions
Both intermittent and continuous energy restriction achieved a comparable effect in promoting weight-loss and metabolic improvements. Long-term trials are needed to draw definitive conclusions.
Background
In the final decade, much interest has been focused on dietary strategies that manipulate energy intake unconventionally, known as intermittent fasting or intermittent free energy restriction (IER) [1,2,3,4]. This dietary arroyo has gained greater attending and popularity as a mode for losing weight alternative to the conventional weight-loss diets, characterized past continuous (non-intermittent) energy restriction (CER). The two most popular forms of IER are: the 5:2 nutrition characterized past two consecutive or non-consecutive "fast" days and the alternate-day free energy restriction, usually chosen alternating-day fasting, alternate-day modified fasting, or every-other-solar day fasting, consisting of a ''fast" mean solar day alternated with a ''feed" day [5]. Commonly, during "fast" days, the free energy intake is severely restricted, ranging from complete abstinence from foods to a daily maximum intake roughly corresponding to 75% energy restriction. Therefore, the term "fast" oftentimes does not involve a true consummate abstinence from caloric intake. The term IER will be used to draw all intermittent free energy-restricted/fasting regimens.
The time-restricted feeding [2, 6,7,viii,9] and the very-low-calorie or energy diets [2, 3] are other types of dietary interventions which were often included in previous systematic reviews and meta-analyses on IER. Indeed, in the erstwhile, individuals are allowed to eat inside a specific range of time, thus, every day there is a menstruation without food intake, varying from 12 to 21 h [10,eleven,12] (i.east. the Muslim Ramadan). On the other manus, there is no daily intermittency in a very-low-calorie-diet, although the overall energy intake may be similar to those of the IER regimens [xiii].
To the best of our knowledge, an overall evaluation of the impact of IER on multiple metabolic variables, on per centum body fat changes, and on the effects of counterbalanced versus ad libitum "feed" days, besides as on the benefits of the unlike "fasting" regimens is at present defective.
The primary objective of this systematic review and meta-assay was to update the efficacy of IER on weight loss, limiting the analyses to regimens which actually included a weekly intermittent energy brake, i.e. from 1 up to 6 "fast days" per week. Furthermore, the impact of IER on fat mass (FM), fatty free mass (FFM), arterial claret pressure (BP) and other cardiometabolic risk factors was assessed. The effects of IER according to the specific blazon of nutritional regimen on all these outcomes were evaluated also.
Materials and methods
Nosotros followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines in the reporting of this study [14].
Search strategy
The post-obit electronic databases were queried using a combination of search terms until the 31th of May 2018: PubMed (National Library of Medicine), the TRIP database, the Cochrane Library, EMBASE, and Cumulative Index to Nursing and Allied Health Literature (CINAHL). The construction of the search strategy was performed using database specific subject headings and keywords. Both medical subject headings (MeSH) and free text search terms were employed. Restrictions to human studies were placed.
The search terms included combinations of "intermittent fasting" or "alternate day fasting" or "intermittent energy restriction" or "periodic fasting", and weight loss, weight gain, obesity, weight, fat mass, claret pressure, blood glucose, insulin, insulin-resistance, insulin sensitivity, glycated hemoglobin A1c (HbA1c), type 2 diabetes mellitus (T2DM), cholesterol, and triglycerides (costless-term and MESH every bit possible) (Additional file 1). These search strategies were implemented by hand searching the references of all the included studies and systematic reviews on the field.
Study pick
We included studies with the following characteristics: (i) randomized controlled trials (RCTs); (2) a detailed description of the IER regimen; (three) 75% of free energy restriction on "fast" days, with a maximum cut-off of 500/660 kcal/day for females/males, respectively; (iv) weekly intermittency of free energy brake (from i up to 6 "fast" days per week); (v) trial duration > 4 weeks; (half-dozen) containing as comparator a group on a CER regimen and (7) including changes in body weight or percent torso weight equally 1 of the report's consequence.
We excluded studies with the following characteristics: (i) uncontrolled trials or written report design other than RCTs; (two) studies not including trunk weight as an upshot and/or defective sufficient information on weight modify; (3) including fourth dimension restricted feeding intervention; (iv) reporting very-low-calorie or fasting regimens for > vi days consecutive/week; and (v) providing > 500–660 kcal/day or not reporting the amount of calorie prescribed on "fast" days.
In trials with multiple interventional arms (i.e. practise arm, intervention arm with specific diets), the IER and the CER artillery were considered, while other arms were non analyzed, since out of the scope of this review.
Ii authors (IC, SB) separately screened abstracts for their inclusion or exclusion; retrieving full text articles from potentially relevant abstracts. Whatever discrepancy virtually inclusion was resolved by discussing with a third author (AE).
Outcomes
The primary outcome of the review was evaluating changes in body weight or in percent body weight. Secondary outcomes were: changes in body mass index (BMI), waist circumference, FM, FFM, arterial BP, and the claret values of fasting glucose and insulin, insulin resistance, insulin sensitivity, HbA1c, full cholesterol, HDL- and LDL-cholesterol, and triglycerides. The changes of these outcomes according to the specific blazon of IER regimen were also evaluated.
Data collection and extraction
From each included study, the following information were extracted (1) offset author proper noun and year of publication; (two) written report design; (three) inclusion criteria of participants; (4) trial duration; (v) number of subjects enrolled in each arm; (half-dozen) blazon of dietary intervention; (7) age, gender, BMI of participants; (8) trunk limerick (FM and FFM); (9) systolic (SBP) and diastolic claret pressure (DBP); (10) blood concentrations of fasting glucose, HbA1c, insulin, full cholesterol, HDL-cholesterol, LDL-cholesterol, and triglycerides; (xi) Homeostasis Model Assessment-Insulin Resistance (HOMA-IR) and insulin-sensitivity alphabetize (Si).
Risk of bias assessment
All studies were independently assessed by two authors (IC, SB) using the "Run a risk of bias" tool adult by the Cochrane Collaboration for RCTs [xv]. The items used for the cess of each study were the post-obit: capability of sequence generation, allotment darkening, blinding, addressing of dropouts (incomplete outcome data), selective outcome reporting, and other potential sources of bias. A judgment of "50" indicated low chance of bias, "H" indicated high risk of bias, and "unclear" indicated an unclear/unknown risk of bias. The possible disagreements were resolved past consensus, or with consultation with a 3rd author (AE).
Information synthesis
Data synthesis was performed but for the outcomes which were reported by > 3 trials.
The pooled effect sizes were expressed equally weighted mean differences (WMD) and 95% confidence interval (CI) betwixt IER and CER arms of the hateful outcome values measured at the end of follow-upward.
The mean difference of changes from baseline was estimated for each study on the footing of reported baseline and follow-up measurements. If the standard deviation for change from baseline was non reported, we imputed missing values assuming a inside-patient correlation from baseline to follow-up measurements of 0.8 as suggested in the Cochrane handbook [16]. When betwixt-arms mean differences on change from baseline were already estimated [17], those information were included. For the relative weight change from baseline, the not-reported standard deviations were imputed using the mean standard deviation of the available studies.
Random-effects models were applied to provide a summary estimate.
Inter-study heterogeneity was assessed using Cochrane Q statistic and quantified by I2 examination [xviii].
Subgroup analyses for all outcomes were performed based on the different dietary regimen of the "feed" days (counterbalanced vs. ad libitum food intake) and the effects of the different regimens of "fasting" (five:2 vs. the other regimens). Weighting of studies was washed using generic inverse variance method.
In order to evaluate the influence of each study on the overall effect size, sensitivity analysis was conducted using the one-written report remove (leave-one-out) approach.
Potential publication bias was explored using visual inspection funnel plot disproportion and Egger's weighted regression tests.
Meta-analyses were performed by using the Stata Metan package (Stata Statistical Software, Release 13; StataCorp LP, College Station, TX); meta-regressions and Egger's weighted regression tests for publication bias were performed using the metafor bundle (version 1.ix-vii) for R (version 3.1.2, R Foundation for Statistical Computing, Vienna, Austria).
Results
Included studies
The initial literature search identified 8577 records. After removing duplicates, 6943 records were screened, and, afterwards excluding manufactures non coming together the inclusion criteria, 94 records were assessed for eligibility. After further analysis and quality assessment, a total of 11 studies were selected for the systematic review and meta-analysis (Fig. ane). All studies identified were RCTs, reporting an IER arm and a CER arm comparison; the corresponding details are shown in Table 1. Information relative to participants involved in exercise-only arms [nineteen] or in high-protein dietary intervention [twenty] were not considered, because not pertinent to the aims of the study.
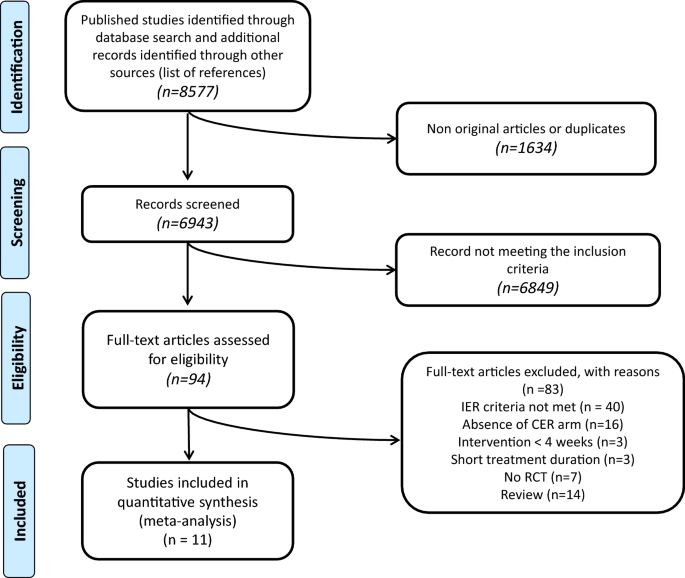
Menstruum of the study
Characteristics of the studies
The total number of subjects included in the present assay was 630 at enrolment. During the grade of the trials, 102 patients dropped out. Drop-out rates ranged from about 2% [21] to 38% for IER artillery [22] and from 0% [23] to l% [22] for CER. The number of participants analyzed at the end of the RCTs was 528.
In that location was a greater number of women among participants, with the exception of 3 studies with a counterbalanced number between men and women [21, 22, 24] and 1 enrolling only men [23]. Participants were individuals with overweight/obesity; in 2 RCTs patients with T2DM were selected [23, 25], and in 1 RCT patients with multiple dysmetabolic conditions were enrolled [21]. In all RCTs except for two [23, 25], participants with a stable weight earlier the commencement of the report, without history of bariatric surgery, and without drugs impacting on weight or the other study outcomes, were studied.
Trials were performed in Britain [20, 22, 26], in United states of america [17, 19, 25, 27], in Australia [23, 24], and Kingdom of norway [21, 28]. The elapsing of the studies ranged from 8 weeks [27] to 24 weeks [17, 21, 23, 26].
Dietary intervention
Four studies prescribed alternating "fast" and "feed" days [17, xix, 27, 28]. Six studies used 2 "fast" days and 5 "feed" days per week (5:2 diet) [21,22,23,24, 26]. In 1 RCT, 5 consecutives "fast" days were prescribed before a one "fast" 24-hour interval/calendar week regimen per 15 weeks in the IER arm, while the other arm (v "fast" days every five weeks) was not considered, since no intermittence inside the same week was present [25]. On "fast" days, diets provided a maximum of 660 kcal/twenty-four hour period. In 2 studies, participants were instructed to consume their meals between 12:00 p.m. and 2:00 p.m. on "fast" days to ensure that subjects underwent the same elapsing of fasting [17, 19]. In 4 studies, meals of "fast" days were partially [17, 25] or totally supplied [19, 27]. In 1 study, a commercially bachelor very-low free energy formula-based food was assigned in the "fast" days [22].
On "feed" days, half-dozen studies prescribed good for you and balanced eating pattern, co-ordinate to the energy requirements [17, 20, 22, 25, 26, 28], 4 immune for ad libitum food intake based on the participants' usual eating [19, 21,22,23,24] and ane provided a diet based on the energy requirements simply allowing the access to 5–vii optional food modules (200 kcal each) [27]. In the comparator arms, energy was restricted by approximately 25% of the daily energy requirements in all studies (CER arms).
Dietary compliance and energy intake cess
6 studies specifically assessed the compliance to the diet and the overall energy intake in both artillery past filling 7-twenty-four hour period nutrient records at dissimilar time points [17, 20,21,22, 26, 28]. In 1 study, dieticians evaluated adherence past using patients' self-recorded dietary diaries and diet histories taken during their dietetic appointments [23]. Either similar adherence between IER and CER [20, 21, 23, 26, 28], a lower [17] or a higher [22] adherence in the IER arms were reported. Adherence to the recommendations in the IER arms ranged from 64% [26] to 93% [22] at the cease of the RCTs, simply information were difficult to compare because of their incompleteness and the dissimilar methods employed to evaluate the compliance.
Take chances of bias assessment
Some of the analyzed trials were characterized by the lack of information about the randomization procedures (Additional file two). If blinding of participants was not feasible owing to the nature of the interventions, data almost blinding of the personnel performing the laboratory or statistical analyses were always unknown, except for ane study [20]. Dropouts were higher in the IER arms [17, 26, 28] or in the CER arms [20, 22, 24, 25], thus introducing a possible option bias between-arms, but intention-to treat analyses were performed past all studies, except for 1 RCT [22], where information of the completers merely have been reported. Finally, most trials appeared to be free of selective upshot reporting and of other sources of bias, autonomously from ane, where body weight at baseline was not reported [xix].
Meta-analysis
All the outcomes of involvement of this systematic review are reported in Additional file 3. Data synthesis was performed for the outcomes reported past > 3 trials, therefore data relative to Si values were not pooled.
Weight loss
All RCTs reported weight loss in the IER artillery during the intervention, ranging from 5.ii% [19] of initial weight to 12.nine% [28], while in the CER arms, changes ranged from four.3% [twenty] to 12.1% [28] (Boosted file 3). Pooled information from random-effect assay did not bear witness a significant effect of IER on weight loss (WMD: − 0.61 kg, 95% CI − 1.70 to 0.47; p = 0.27) (Fig. 2). The estimated upshot on trunk weight did not modify in the get out-one-out sensitivity analysis (data not shown).
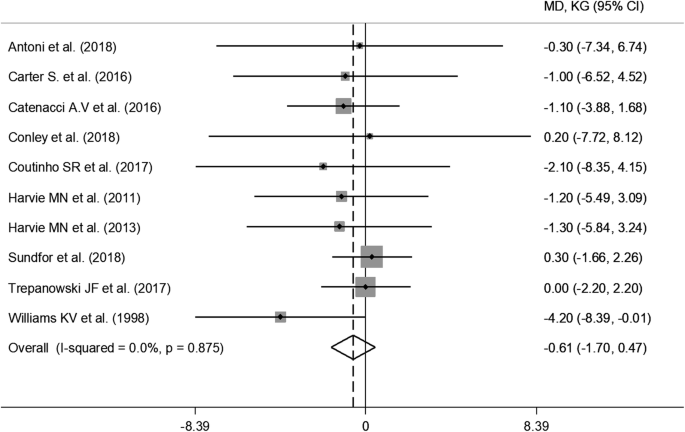
Meta-assay of the furnishings of intermittent energy restriction versus continuous energy brake on weight loss. MD (hateful difference) indicates the hateful departure on change from baseline of the IER vs. the CER arms. The plotted points are the mean differences and the horizontal error bars represent the 95% confidence intervals. The grey areas are proportional to the weight of each written report in the random-effects meta-analysis. The vertical dashed line represents the pooled point estimate of the mean difference. The solid black line indicates the goose egg hypothesis (MD = 0)
Subgroup analyses based on the type of regimen (5:2 vs. other regimens) as well as on the dietary characteristics of the "feed" days of the IER interventions (advertizement libitum vs. balanced food intake) showed consistent results, every bit reported in Additional file four. Analyses were repeated later on the exclusion of the trial prescribing v consecutives "fast" days so ane "fast" day/week per 15 weeks [25], and the results did not modify (WMD: − 0.36 kg, 95% CI − one.48 to 0.77; p = 0.54). Finally, the RCT reporting the percentage relative variations of the endpoints merely [19] was included in the analyses, and the estimated effect size of weight change did not bear witness whatever betwixt-arms difference (WMD: − 0.08, 95% CI − 0.23 to 0.07; p = 0.29).
Similarly, the percent weight loss was like in both arms (WMD: − 0.38%, 95% CI − one.xvi to 0.40; p = 0.34) and the results did not differ either in the subgroup analyses (Additional file v) or in the leave-1-out sensitivity analysis.
Other anthropometric measures
7 out of the 11 included RCTs reported changes in FM and FFM [17, xx, 22, 24, 26,27,28]. FM was measured by unlike methods: body impedance analysis (BIA) [20, 22]; dual X-ray absorptiometry (DXA) [17, 24, 27]; impedance [26]; air displacement plethysmography [28]. Pooled results showed no departure between-artillery in FM (WMD: − 0.23 kg, 95% CI − 1.23 to 0.77; p = 0.66) equally well as in FFM (WMD: − 0.22 kg, 95% CI − one.01 to 0.56; p = 0.58), equally shown in Boosted file half dozen. Those results were consistent both at subgroup analyses and at sensitivity analyses. Five RCTs assessed waist circumference [20,21,22,23, 26] without showing any differences between arms (WMD: − 0.17 cm; 95% CI − 1.74 to 1.39; p = 0.83).
Cardiometabolic biomarkers
Pooled information obtained from glucose, HbA1c, insulin and HOMA-IR are presented in Fig. 3a–d respectively. Changes in fasting glucose and HbA1c values were reported respectively in 7 [17, xx,21,22,23, 26, 27] and four [21, 24,25,26] trials. Random-effect analysis showed no difference either on glucose (WMD: − 0.49 mg/dL, 95% CI − 1.98 to 0.99; p = 0.51) or HbA1c (WMD: − 0.02%, 95% CI − 0.10 to 0.06; p = 0.62) changes in the IER when compared to CER arms with consistent results in subgroup/sensitivity analyses.
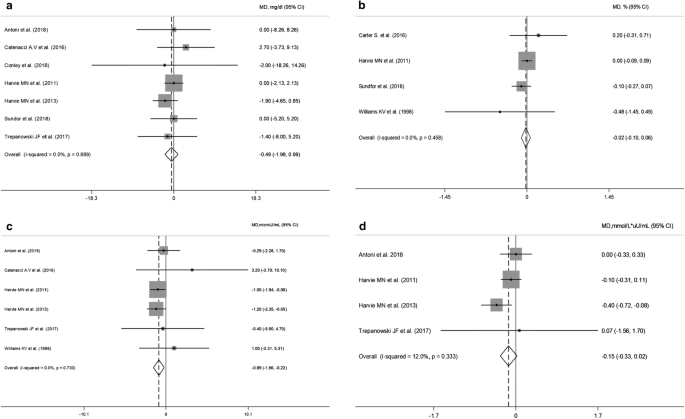
Meta-analysis of the effects of intermittent energy restriction versus continuous energy restriction on fasting glucose (a), HbA1c (b), insulin (c) and HOMA-IR (d) values. Md (hateful difference) indicates the mean difference on modify from baseline of the IER vs. the CER arms. The plotted points are the mean differences and the horizontal error confined represent the 95% conviction intervals. The grey areas are proportional to the weight of each study in the random-effects meta-analysis. The vertical dashed line represents the pooled point estimate of the mean deviation. The solid black line indicates the cypher hypothesis (Doc = 0)
On the contrary, fasting insulin values were significantly reduced with IER (WMD = − 0.89 µU/mL; 95% CI − 1.56 to − 0.22; p = 0.009; I2 = 0%) and the estimated event appeared robust in the leave-one-out sensitivity analysis (data non shown). Moreover, subgroup analyses showed that the v:2 regimens were associated with increased insulin reductions (WMD: − 0.99 µU/mL; 95% CI − 1.67 to − 0.30; p = 0.005; I2 = 0) (Additional file 7). All the RCTs evaluating fasting insulin values included a balanced energy regimen for the "feed" days. HOMA-IR values were reduced, though not significantly, in the IER regimens (WMD = − 0.xv mmol/50 × µU/mL; 95% CI − 0.33 to 0.02; p = 0.09).
Just 1 RCT evaluated insulin sensitivity (Si) past a frequently sampled intravenous glucose tolerance [21], without betwixt-artillery differences.
Pooled data obtained from viii RCTs [17, twenty,21,22,23, 25,26,27] did not show any pregnant effect of IER on triglyceride concentrations (WMD: − 3.11 mg/dL, 95% CI − 9.76 to 3.54; p = 0.36) (Fig. 4a). However, subgroup analyses showed a slightly significant triglyceride reduction in the IER artillery employing other fasting regimens (WMD = − xiv.4 mg/dL 95% CI − 28.6 to − 0.23; p = 0.046; Itwo = 0%). Characteristics of the "feed" days were not associated with differences in triglyceride changes (Additional file 8). HDL-cholesterol levels increased after IER regimens, admitting not significantly (WMD = i.72 mg/dL 95% CI − 0.20 to iii.63; p = 0.07) (Fig. 4c). Subgroup analysis revealed a significant HDL-cholesterol increase with a balanced diet on "feed" days (WMD = 2.88 mg/dL 95% CI 0.66 to 5.09; p = 0.011; I2 = 0%) compared with advertizing libitum eating (Additional file ix). No between-arm differences were institute for full cholesterol and LDL-cholesterol (Fig. 4b, d). Finally, changes in both SBP and DBP did not significantly differ between arms (Additional file 10).
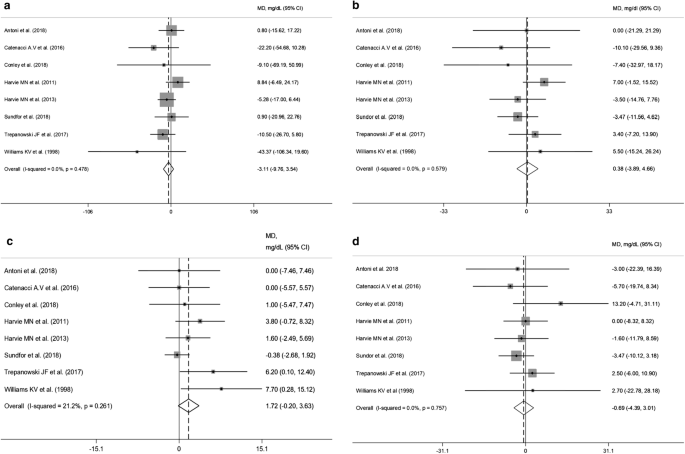
Meta-assay of the effects of intermittent energy restriction versus continuous energy restriction on triglycerides (a), total cholesterol (b), HDL-cholesterol (c) and LDL-cholesterol (d) values. MD (mean difference) indicates the mean difference on modify from baseline of the IER vs. the CER arms. The plotted points are the hateful differences and the horizontal error confined represent the 95% conviction intervals. The grey areas are proportional to the weight of each study in the random-effects meta-analysis. The vertical dashed line represents the pooled signal estimate of the mean difference. The solid black line indicates the null hypothesis (Medico = 0)
Publication bias
We used the Egger's test for funnel plot disproportion to detect a potential publication bias on reporting results on weight alter. Exam result (p = 0.15) did not propose whatsoever asymmetry in the funnel plot (Additional file 11).
Prophylactic
No major adverse events were reported. Only 1 patient from the IER arm of the RCT supplying 0 kcal during "fast" days developed gallbladder dyskinesia and underwent cholecystectomy after completing the written report, but this event was reported to exist unrelated to the intervention [27]. Minor physical or psychological adverse effects, such as lack of energy, headaches, feeling common cold, constipation, bad breath, lack of concentration, bad atmosphere, were reported in a minority of participants from the IER arms (< 20%) in a few studies [20, 21, 23, 26]. On the other hand, hunger was reported in the showtime weeks by well-nigh half of participants to a v:2 regimen in 1 trial, but this symptom improved over time [23].
Give-and-take
An intermittent regimen of energy brake (at least 1 day/week) determined a loss in body weight and pct torso weight similar to continuous (not-intermittent) energy brake. Interestingly, a slight reduction in fasting insulin concentrations was evident with IER regimens employing 2 days/week "fast", just the clinical relevance of this outcome is uncertain.
Furnishings of IER on weight loss and fat mass
Virtually systematic reviews and meta-analyses demonstrated that IER regimens achieved comparable weight loss equally CER regimens [4, five, 9], reporting an overall weight loss ranging from 4 to 8% [2, 3, 7, 9], and a difference of − 4.14 kg to + 0.08 kg versus the comparator artillery [iv, 5, 29]. Our results are in accordance, even if the trials previously included differed from ours, since we have included only RCTs with a at to the lowest degree 1 solar day/week and no more than vi twenty-four hours/week of "fasting", and with an extremely low energy supply during the "fast" days. This latter choice derived from the idea of studying conditions simulating as much as possible a condition of fasting, whose benefits, proven by animal studies, seem to depend on the shift in metabolism from glucose utilization and fat synthesis/storage towards reduced insulin secretion and fatty mobilization/oxidation [xxx, 31].
In that location is no articulate definition of IER, and intermittent regimens providing upwards to 800 kcal [5, 9], with ≥ seven "fast" days [4, 6, 9, 29], including time-restricted feeding [2, 6,7,eight, 32], with unlimited energy restriction as a comparator group [ii, 3, five,half dozen,seven], or not randomized controlled trials [ii] have been included within previous reviews. We have taken care to define precise inclusion criteria to limit variability and increase the comparability amidst trials, and nosotros have obtained a low heterogeneity.
It could exist hypothesized that the very low caloric intake on "fast" days adamant an overall lower caloric intake in the IER arms, which were therefore difficult to be compared with the CER arms. In the but RCT where water and calorie-free beverages were immune in the "fast" days, a significant between-artillery difference in energy intake was axiomatic [27]; in two studies a between-arms difference of 300–400 kcal was observed [22, 23] while almost RCTs reported a negligible between-arms difference (~ 100 kcal) [17, 20, 21, 25, 26]. Consistently, our sensitivity and subgroup analyses did not observe meaning between-arms differences.
Furthermore, the per centum weight loss was highly overlapping, and no apparent superiority of a dietary regimen was axiomatic. Indeed, participants of the IER arms from all RCTs lost ≥ 5% of their initial weights, thus confirming the clinical usefulness of this arroyo at least in the short term, i.e. inside 24 weeks.
Previous reviews reported a FM loss ranging from 4 to seven% [three] to xi–16% [two] in the IER artillery, and the just meta-analysis evaluating this outcome reported a differential loss of 1.38 kg with respect to comparator arms [five]. We failed to detect significant betwixt-artillery difference for this outcome, suggesting that such a regimen could be a valid, but non superior alternative to CER.
Intriguingly, participants to the IER regimens usually did not swallow as much food in the "feed" days as to compensate for the caloric brake of the "fast" days, thus suggesting that IER could reduce food intake even in the "feed" days, without compensatory overeating [6, 31]. This finding was not confirmed by all studies [28, 33, 34]. Furthermore, adverse events were sometimes college with the IER regimens [xx, 21, 26], and the participants reported stronger feelings of hunger [21, 23]. The compliance and adherence to the intervention diets was heterogeneous among trials, the attrition rate was often higher in the IER arms [17, 22, 24, 26, 31, 35], and the percentage of participants planning to continue with the dietary regimen beyond 6 months was lower in the IER arms [26]. Overall, these data practise not support the fact that IER is easier and more adequate than CER to everyone. Moreover, the reduction in resting free energy expenditure, i.e. the compensatory metabolic response which reduces the degree of weight loss, has been reported to be either reduced (favoring weight loss) [27, 36] or increased (attenuating weight loss) [22, 28] with IER regimens. Indeed, some studies suggest that IER evokes the aforementioned adaptive response every bit CER [6, 37].
The hypothesized benefits of IER, extensively studied in animate being models, included the use of fats during severe free energy restriction with preferential reduction of adipose mass, the stimulation of browning in white adipose tissue, increased insulin sensitivity, lowering of leptin and increased human growth hormone, ghrelin and adiponectin circulating levels, reduced inflammation and oxidative stress [30]. The trigger of adaptive prison cell response leading to enhanced ability to cope with stress, improved autophagy by sirtuin-1 activity stimulation, modification of apoptosis, increase of vascular endothelial growth factor expression in white adipose tissue, the action on the metabolism via Forkhead Box A genes, and reduction of advance glycation end-products might be all possible metabolic pathways explaining the beneficial effects of IER [7, 30, 38, 39]. In mice, IER adamant metabolic improvements and weight loss as a consequence of a shift in the gut microbiota limerick, leading to an increase in the production of acetate and lactate and to the selective upregulation of monocarboxylate transporter in beige adipose cells which stimulate biscuit fat thermogenesis [40]. At present, many of these adaptive mechanisms have been demonstrated in animal experimental models merely not in humans, thus more research is still needed.
Effects of IER on cardiometabolic markers
IER regimens were associated with lower circulating insulin values; a significant reduction was axiomatic for the five:two "fasting" regimen only. Indeed, two RCTs, both employing this regimen, determined the departure [xx, 26]. Our data are in line with the results of a previous meta-assay reporting a significantly higher reduction in fasting insulin (− 0.67 µU/mL) in the IER arms [5]. The difference we found (− 0.89 µU/mL) was statistically significant, just not clinically relevant, above all considering the fact that participants to the included RCTs were overweight/obese and therefore probably insulin-resistant individuals.
Our data synthesis on glucose, HOMA-IR, HbA1c showed no between-arms difference. We did not include patients with T2DM from 2 RCTS in the pooled analysis on fasting glucose, since most participants were on hypoglycemic drugs and their glycemic values would be certainly influenced past the treatment [24, 25]. Highly contrasting human studies are available almost the benefits of IER on glucose metabolism and insulin sensitivity [iii, vi, 31], contrarily to animal studies strongly suggesting a benefit in T2DM prevention [one, 31]. The improvements in glucose homeostasis might be therefore comparable to those obtained by continuous energy restrictions.
Our meta-assay did non show significant between-arms difference in lipid values and arterial blood pressure, with the exception of a pocket-size difference in subgroup analyses on triglyceride concentrations (− 14 mg/dL) and HDL-cholesterol (+ 2.88 mg/dL), non meaningful from a clinical indicate of view. Almost studies showed reduction in triglyceride levels between 15 and 42% in the IER arms [31, 41], and the but available meta-analysis reported a between-arms not significant difference of two.65 mg/dL [v]. Reduction in full cholesterol, LDL-cholesterol in the IER arms ranged respectively between half dozen–25%, 7–32%, with small effects on HDL-cholesterol [1, 31], and between-arms differences resulted not pregnant [five]. Intriguingly, a few studies reported that IER regimens determined an increment in LDL particle size [xix, 42], and reduced post-prandial hypertriglyceridemia [22], thus potentially conferring cardio-protection, since the lower the LDL size, the higher the oxidizability and the susceptibility to arterial penetration, and college post-prandial hyperlipemia is a mark of atherosclerosis progression. Furthermore, fasting can human activity on many enzymes implicated in lipid and lipoprotein metabolism [27]. Notwithstanding, all these reports need confirmation in larger human RCTs.
Similarly, data on arterial BP were controversial, with the majority of human studies reporting no differences between IER and CER regimens [i, 5, 31, 41]. Indeed, most of the published studies and RCTs included normotensive subjects at baseline, making it hard to identify differences between-artillery.
Therefore, unlike the very promising data on animals, evidence is not sufficiently robust to suggest the superiority of intermittent vs. continuous caloric restriction regimens on the main cardiovascular factors in humans.
Clinical implications
Weight loss maintenance should be an integral component of the management of obesity, attributable to the weight regain usually occurring with time. The two RCTs including longer follow-ups (24 months) did not find between-arms differences in weight loss maintenance [17, 27]. Studies with longer follow-ups, evaluating the long-term sustainability, adherence to, and rubber of IER regimens are needed. Furthermore, no RCT evaluated difficult endpoints, such every bit cardiovascular outcomes or T2DM incidence. Two observational cohort studies found that fasting was associated with a lower prevalence of coronary avenue diseases or diabetes diagnosis but are limited by a lack of a comprehensive dietary history and many potential bias [43, 44]. Information technology could exist hypothesized that IER regimens should exist proposed in clinical practice, since it is possible that some individuals observe easier to reduce their energy intakes for i or more days per week, rather than every twenty-four hour period. It is well known that a single diet fit not all, and in the choice of the private's tailored regimen, IER strategies should be considered past health care professionals. In this way, information on the feasibility of these regimens in "real life" would exist obtained.
Strengths and limitations
This is, to our noesis, the largest and updated meta-assay on the effects of IER on weight loss and multiple metabolic outcomes, setting strict inclusion criteria to increase comparability among studies.
The high variability among the RCTs in the feeding protocols, the limited follow-upward, the small sample sizes, the loftier drop-out rates potentially leading to selection bias, the limited reporting of adverse events and blinding of investigators virtually arm resource allotment, or other methodological problems are all limitations to exist considered. Finally, most studies were performed by the same authors and the majority of subjects included were adult healthy women, thus limiting the generalizability of the results.
Conclusion
In overweight/obese adults, IER is equally effective equally CER for promoting weight loss and metabolic improvements in the short term. Further long-term investigations are needed to draw definitive conclusions.
Abbreviations
- BIA:
-
body impedance analysis
- BMI:
-
body mass index
- BP:
-
claret pressure
- CER:
-
continuous free energy restriction
- CI:
-
confidence interval
- CINAHL:
-
Cumulative Index to Nursing and Centrolineal Health Literature
- DBP:
-
diastolic blood pressure
- DXA:
-
dual X-ray absorptiometry
- FFM:
-
fat free mass
- FM:
-
fat mass
- HbA1c:
-
glycated hemoglobin A1c
- HOMA-IR:
-
Homeostasis Model Assessment-Insulin Resistance
- IER:
-
intermittent free energy restriction
- MeSH:
-
medical subject field headings
- RCTs:
-
randomized controlled trials
- Si:
-
insulin-sensitivity alphabetize
- SBP:
-
systolic blood force per unit area
- T2DM:
-
type 2 diabetes mellitus
- WMD:
-
weight mean departure
References
-
Varady KA, Hellerstein MK. Alternating-day fasting and chronic affliction prevention: a review of human and beast trials. Am J Clin Nutr. 2007;86:seven.
-
Varady KA. Intermittent versus daily calorie restriction: which diet regimen is more than effective for weight loss? Obes Rev. 2011;12:593.
-
Barnosky AR, Hoddy KK, Unterman TG, Varady KA. Intermittent fasting vs daily calorie brake for type 2 diabetes prevention: a review of human findings. Transl Res. 2014;164:302.
-
Headland M, Clifton PM, Carter S, Keogh JB. Weight-loss outcomes: a systematic review and meta-analysis of intermittent free energy restriction trials lasting a minimum of vi months. Nutrients. 2016;viii:8.
-
Harris L, Hamilton Due south, Azevedo LB, Olajide J, De Brún C, Waller Thousand, et al. Intermittent fasting interventions for handling of overweight and obesity in adults: a systematic review and meta-assay. JBI Database Syst Rev Implement Rep. 2018;16:507.
-
Seimon RV, Roekenes JA, Zibellini J, Zhu B, Gibson AA, Hills AP, et al. Exercise intermittent diets provide physiological benefits over continuous diets for weight loss? A systematic review of clinical trials. Mol Jail cell Endocrinol. 2015;418:153.
-
Horne BD, Muhlestein JB, Anderson JL. Wellness effects of intermittent fasting: hormesis or harm? A systematic review. Am J Clin Nutr. 2015;102:464.
-
Varady KA. Impact of intermittent fasting on glucose homeostasis. Curr Opin Clin Nutr Metab Care. 2016;19:300.
-
Davis CS, Clarke RE, Coulter SN, et al. Intermittent energy restriction and weight loss: a systematic review. Eur J Clin Nutr. 2016;70:292.
-
Rothschild J, Hoddy KK, Jambazian P, Varady KA. Time-restricted feeding and risk of metabolic disease: a review of homo and brute studies. Nutr Rev. 2014;72:308.
-
Patterson RE, Laughlin GA, LaCroix AZ, Hartman SJ, Natarajan L, Senger CM, et al. Intermittent fasting and human metabolic health. J Acad Nutr Nutrition. 2015;115:1203.
-
Hutchison AT, Heilbronn LK. Metabolic impacts of altering meal frequency and timing—does when we eat thing? Biochimie. 2016;124:187.
-
Lantz H, Peltonen M, Agren Fifty, Torgerson JS. Intermittent versus on-demand use of a very depression calorie diet: a randomized 2-year clinical trial. J Intern Med. 2003;253:463.
-
Moher D, Liberati A, Tetzlaff J, Grouping P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA argument. PLoS Med. 2009;half-dozen:e1000097. https://doi.org/ten.1371/journal.pmed.1000097.
-
Higgins JP, Altman DG, Gotzsche PC, Jüni P, Moher D, Oxman AD, et al. The Cochrane Collaboration'due south tool for assessing take a chance of bias in randomised trials. BMJ. 2011;343:5928.
-
Higgins JPT, Light-green S (editors). Cochrane handbook for systematic reviews of interventions version 5.one.0 [updated March 2011]. The Cochrane Collaboration; 2011.
-
Trepanowski JF, Kroeger CM, Barnosky A, Klempel MC, Bhutani Southward, Hoddy KK, et al. Effect of alternating-solar day fasting on weight loss, weight maintenance, and cardioprotection among metabolically good for you obese adults: a randomized clinical trial. JAMA Intern Med. 2017;177:930.
-
Higgins J, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. Br Med J. 2003;327:557.
-
Varady KA, Bhutani S, Klempel MC, Kroeger CM. Comparison of furnishings of diet versus practice weight loss regimens on LDL and HDL particle size in obese adults. Lipids Wellness Dis. 2011;10:119.
-
Harvie M, Wright C, Pegington M, McMullan D, Mitchell Due east, Martin B, et al. The effect of intermittent energy and carbohydrate restriction 5. daily free energy restriction on weight loss and metabolic illness gamble markers in overweight women. Br J Nutr. 2013;110:1534.
-
Sundfør TM, Svendsen Grand, Tonstad Due south. Effect of intermittent versus continuous energy restriction on weight loss, maintenance and cardiometabolic risk: a randomized ane-year trial. Nutr Metab Cardiovasc Dis. 2018;28:698.
-
Antoni R, Johnston KL, Collins AL, Robertson MD. Intermittent v. continuous free energy brake: differential effects on postprandial glucose and lipid metabolism following matched weight loss in overweight/obese participants. Br J Nutr. 2018;119:507.
-
Conley Grand, Le Fevre L, Haywood C, Proietto J. Is ii days of intermittent energy restriction per week a viable weight loss approach in obese males? A randomised pilot study. Nutr Diet. 2018;75:65.
-
Carter S, Clifton PM, Keogh JB. The effects of intermittent compared to continuous energy restriction on glycaemic control in blazon 2 diabetes; a pragmatic pilot trial. Diab Res Clin Pract. 2016;122:106.
-
Williams KV, Mullen ML, Kelley DE, Wing RR. The event of short periods of caloric brake on weight loss and glycemic command in type 2 diabetes. Diab Intendance. 1998;21:2.
-
Harvie MN, Pegington Thou, Mattson MP, Frystyk J, Dillon B, Evans 1000, et al. The effects of intermittent or continuous energy restriction on weight loss and metabolic illness adventure markers: a randomized trial in young overweight women. Int J Obes. 2011;35:714.
-
Catenacci VA, Pan Z, Ostendorf D, Brannon S, Gozansky WS, Mattson MP, et al. A randomized pilot study comparing nix-calorie alternate-day fasting to daily caloric brake in adults with obesity. Obesity. 2016;24:1874.
-
Coutinho SR, Halset EH, Gåsbakk S, Rehfeld JF, Kulseng B, Truby H, et al. Compensatory mechanisms activated with intermittent energy restriction: a randomized control trial. Clin Nutr. 2018;37:815.
-
Harris L, McGarty A, Hutchison Fifty, Ells L, Hankey C. Curt-term intermittent energy brake interventions for weight management: a systematic review and meta-analysis. Obes Rev. 2018;19:1.
-
Longo VD, Mattson MP. Fasting: molecular mechanisms and clinical applications. Cell Metab. 2014;19:181.
-
Anton SD, Moehl K, Donahoo WT, Marosi One thousand, Lee SA, Mainous AG third, et al. Flipping the metabolic switch: understanding and applying the wellness benefits of fasting. Obesity. 2018;26:254.
-
Santos HO, Macedo RCO. Impact of intermittent fasting on the lipid profile: assessment associated with diet and weight loss. Clin Nutr ESPEN. 2018;24:xiv.
-
Heilbronn LK, Smith SR, Martin CK, Anton SD, Ravussin E. Alternating-day fasting in nonobese subjects: effects on body weight, trunk composition, and energy metabolism. Am J Clin Nutr. 2005;81:69.
-
Arguin H, Dionne IJ, Sénéchal M, Bouchard DR, Carpentier Air-conditioning, Ardilouze JL, et al. Short- and long-term effects of continuous versus intermittent restrictive diet approaches on body limerick and the metabolic profile in overweight and obese postmenopausal women: a airplane pilot study. Menopause. 2012;19:870.
-
Horne BD. Is periodic fasting really good for reducing cardiovascular take chances and improving eye health? Fut Cardiol. 2011;7:721.
-
Byrne NM, Sainsbury A, King NA, Hills AP, Wood RE. Intermittent energy brake improves weight loss efficiency in obese men: the MATADOR study. Int J Obes. 2018;42:129.
-
Harvie M, Howell A. Potential benefits and harms of intermittent free energy brake and intermittent fasting amongst obese, overweight and normal weight subjects—a narrative review of human and creature evidence. Behav Sci. 2017;xix:vii.
-
Golbidi S, Daiber A, Korac B, Li H, Essop MF, Laher I. Health benefits of fasting and caloric restriction. Curr Diab Rep. 2017;17:123.
-
Kim KH, Kim YH, Son JE, Lee JH, Kim Southward, Choe MS, et al. Intermittent fasting promotes adipose thermogenesis and metabolic homeostasis via VEGF-mediated culling activation of macrophage. Jail cell Res. 2017;27:1309.
-
Li G, Xie C, Lu Due south, Tian Y, Li Fifty, Patel D, et al. Intermittent fasting promotes white adipose browning and decreases obesity by shaping the gut microbiota. Cell Metab. 2017;26:672.
-
Johnstone A. Fasting for weight loss: an effective strategy or latest dieting trend? Int J Obes. 2015;39:727.
-
Klempel MC, Kroeger CM, Varady KA. Alternate twenty-four hour period fasting increases LDL particle size independently of dietary fat content in obese humans. Eur J Clin Nutr. 2013;67:783.
-
Horne BD, May HT, Anderson JL, Kfoury AG, Bailey BM, McClure BS, Intermountain Center Collaborative Study, et al. Usefulness of routine periodic fasting to lower risk of coronary artery illness in patients undergoing coronary angiography. Am J Cardiol. 2008;102:814.
-
Horne BD, Muhlestein JB, May HT, Carlquist JF, Lappé DL, Bair TL, Intermountain Centre Collaborative Report Group, et al. Relation of routine, periodic fasting to risk of diabetes mellitus, and coronary artery disease in patients undergoing coronary angiography. Am J Cardiol. 2012;109:1558.
Authors' contributions
IC participated in the formulation and design of the study, information collection and revision, estimation of the findings of the study, manuscript writing and revision. AE participated in the data analysis, interpretation of the findings, manuscript writing and revision. VP, GC participated in the data analysis, interpretation of the findings, and manuscript revision. LSo, LSa, FP, FC, EG participated in the interpretation of the findings, and manuscript revision. SB participated in the conception and design of the study, data drove and revision, manuscript writing and revision. All authors read and canonical the final manuscript.
Acknowledgements
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Availability of information and materials
All information analyzed during this study are included in this published article.
Consent for publication
Non applicable.
Ethics approval and consent to participate
Not applicative.
Funding
Not applicable.
Publisher'south Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Author information
Affiliations
Corresponding author
Boosted files
Additional file i.
Electronic search strategy.
Additional file 2.
Risk of bias assessment in the trials included in the systematic review.
Boosted file 3.
Changes in outcomes at the finish of the trials.
Additional file iv.
Subgroup analysis of weight loss based on the type of regimen (a) and on dietary characteristics of the "feed" days (b).
Additional file v.
Pct weight loss (a) and subgroup assay of percent weight loss based on the blazon of regimen (b) and dietary characteristics of the "feed" days (c).
Boosted file vi.
Meta-analysis of the effects of intermittent energy restriction versus continuous energy restriction on torso composition (a) and waist circumference (b).
Additional file 7.
Subgroup analysis of fasting insulin based on the type of regimen.
Additional file 8.
Subgroup assay of triglycerides based on the type of regimen (a) and dietary characteristics of the "feed" days (b).
Additional file ix.
Subgroup assay of HDL-cholesterol based on the type of regimen (a) and dietary characteristics of the "feed" days (b).
Additional file 10.
Meta-analysis of the furnishings of intermittent energy restriction versus continuous energy restriction on systolic blood pressure (SBP) (a) and diastolic blood force per unit area (DBP) (b).
Additional file 11.
Funnel plot for publication bias detection on weight loss changes.
Rights and permissions
Open Access This article is distributed nether the terms of the Creative Eatables Attribution four.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted utilise, distribution, and reproduction in whatsoever medium, provided y'all give appropriate credit to the original author(due south) and the source, provide a link to the Artistic Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/one.0/) applies to the information made available in this commodity, unless otherwise stated.
Reprints and Permissions
About this commodity
Cite this article
Cioffi, I., Evangelista, A., Ponzo, Five. et al. Intermittent versus continuous energy restriction on weight loss and cardiometabolic outcomes: a systematic review and meta-analysis of randomized controlled trials. J Transl Med 16, 371 (2018). https://doi.org/10.1186/s12967-018-1748-four
-
Received:
-
Accustomed:
-
Published:
-
DOI : https://doi.org/x.1186/s12967-018-1748-4
Keywords
- Continuous free energy restriction
- Intermittent energy restriction
- Fasting glucose
- Triglycerides
- Weight loss
smithmarjohishe00.blogspot.com
Source: https://translational-medicine.biomedcentral.com/articles/10.1186/s12967-018-1748-4
0 Response to "Intermittent Energy Restriction and Weight Loss a Systematic Review"
Post a Comment